A practical guide for healthcare organizations navigating financial, time and resource constraints.
Every healthcare organization feels the pressure of limited resources.
For some, it’s a complex enterprise budget with competing priorities across departments. For others, it’s a lean team balancing patient care with administrative work. And for many, especially grant-funded organizations, every dollar is already spoken for.
So, when contract lifecycle management (CLM) enters the conversation, the response is often the same: We don’t have the budget for that.
But here’s the reality, most organizations already have a contract budget. It’s just hidden in inefficiencies, delays and avoidable risk.
The budget you don’t see.
Budget isn’t just about dollars allocated in a line item. In healthcare, it shows up in three places:
-
Financial budget
-
Time budget
-
Risk budget
And across organizations of every size, contracts are quietly consuming all three.

Research shows organizations lose up to 9% of annual revenue due to poor contract management.* That loss doesn’t appear in a budget report, but it’s very real.
The cost looks different depending on where you sit.
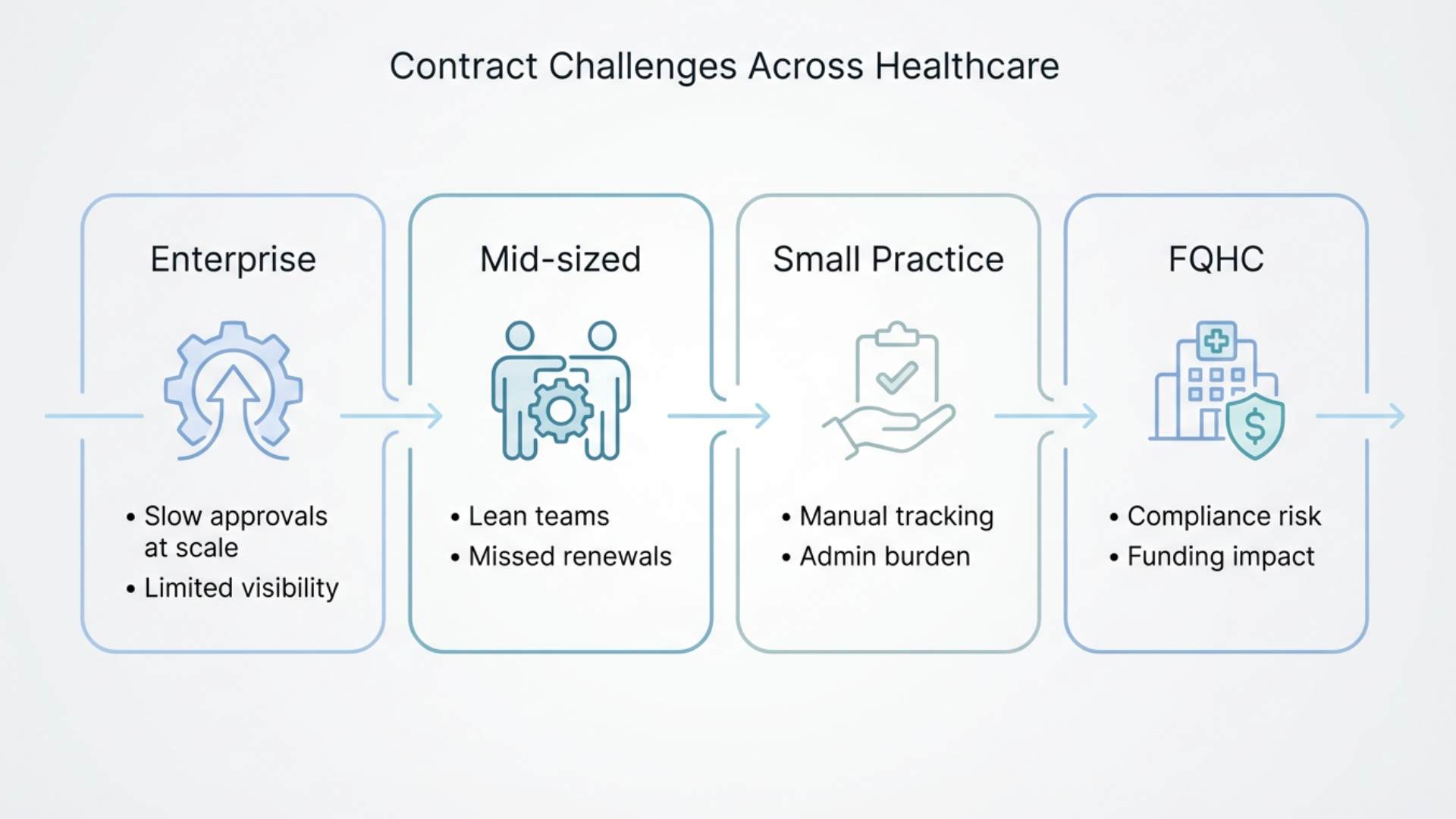
The challenge is shared, the impact however, is not.
In large health systems, contract inefficiencies slow down initiatives at scale. A delay in approvals or lack of visibility can affect thousands of agreements and millions in revenue.
In mid-sized and regional organizations, lean teams carry the burden. Contracts compete with every other operational priority, leading to missed deadlines and slower turnaround times.
In smaller practices and specialty groups, contracts are often managed reactively. Providers and administrators spend valuable time tracking agreements instead of focusing on care and growth.
In FQHCs and grant-funded organizations, the stakes are even higher. Contract mismanagement can impact compliance, reporting and future funding eligibility. Every decision must reflect responsible stewardship of limited resources.
What CLM actually gives back.
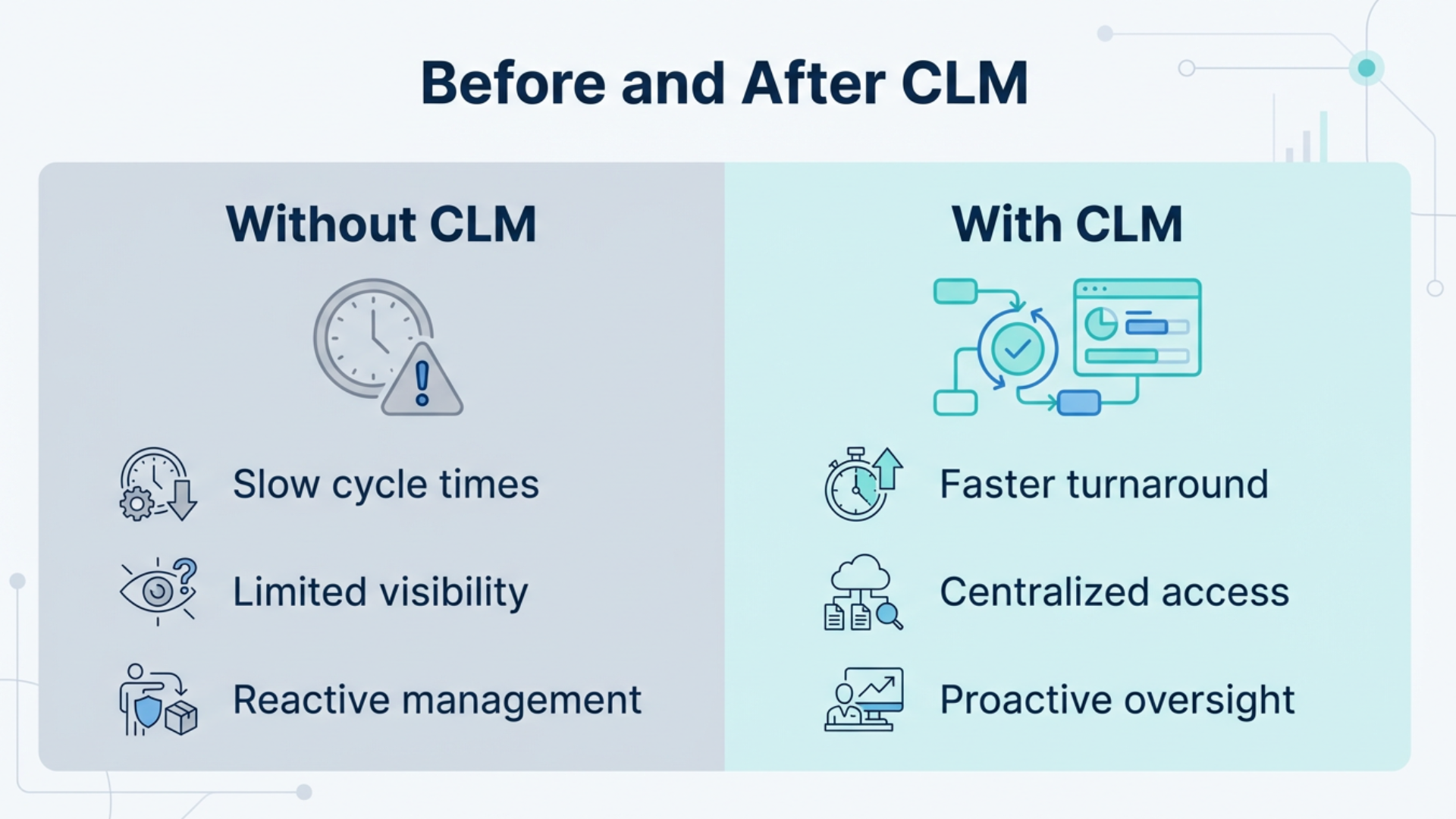
When organizations evaluate CLM, the focus often lands on cost.
What gets overlooked is what it returns.
CLM can deliver measurable impact across the same three budget areas.
-
Reduce contract cycle times by up to 50%**
-
Improve visibility into obligations and renewals
-
Decrease reliance on manual processes and outside counsel
-
Recover lost revenue tied to missed or under-managed contracts
Some studies show CLM solutions delivering 300% or more in return on investment, with even higher returns in high-growth environments.***
Finding the budget based on your reality.
There’s no single path to making CLM work, but there are practical ways organizations make room for it.
If you’re in a large health system:
Look for overlap and inefficiency across departments. Multiple teams managing contracts in different ways often leads to duplicated effort and unnecessary spend. Consolidation alone can unlock meaningful budget.
If you’re in a mid-sized or regional organization:
Start with a focused use case. Renewals, intake or repository management can create immediate impact without requiring a full transformation upfront.
If you’re a smaller practice or specialty group:
Focus on time savings. The ability to reduce manual tracking and follow-up can free up staff to focus on higher-value work. In many cases, time recovered is just as important as dollars saved.
If you’re a grant-funded or mission-driven organization:
Frame CLM as a tool for accountability. Improved visibility and tracking support compliance and demonstrate responsible use of funding. That’s not just operationally beneficial, it’s mission-critical.

Building the case internally.
Getting buy-in often requires reframing the conversation.
Instead of asking for a new budget, start by quantifying what contracts are already costing.
-
How much time is spent managing contracts today?
-
How many renewals are missed or delayed?
-
Where is revenue slowing due to contract bottlenecks?
-
What risks exist due to lack of visibility?
Even simple estimates can shift the conversation from cost to opportunity.
![]()
The shift that changes everything.
The biggest barrier to CLM isn’t budget, it’s visibility.
When organizations can clearly see how contracts impact time, revenue and risk, the conversation changes.
CLM is no longer an added expense. It becomes a way to protect resources, support teams and strengthen operations across the organization.
That looks different in every healthcare setting, but the outcome is the same.
More clarity, more control and better use of what you already have.
Sources:
*World Commerce & Contracting (formerly IACCM), “The Impact of Poor Contract Management,” estimating average value erosion of 8.6% across contracts.
** World Commerce & Contracting (formerly IACCM), research indicating that improved contract management processes can reduce cycle times by up to 50%.
*** Forrester Consulting, “The Total Economic Impact of Contract Lifecycle Management,” reporting significant ROI, often exceeding 300% depending on implementation and scope.




![[Podcast] Highway to Health: “Contract Life Cycle Management is Coming Out on Top, as Healthcare Providers Increasingly Rely on the Tool”](https://www.ntracts.com/hs-fs/hubfs/Imported_Blog_Media/Podcast-Thumbnail.jpg?width=352&name=Podcast-Thumbnail.jpg)